Go With Your Gut
July 5, 2021Recent findings from the Weizmann Institute identify how the Mediterranean diet in relation to gut health paves the way for medical advances, all the while providing a sustainable nutritional lifestyle.
There’s an old saying that the way to one’s heart is through their stomach, and today, the way to a healthier quality of life is quite literally by way of the stomach as well. Israel is well known for being one of the world’s healthiest countries, all thanks to the country’s Mediterranean dietary options. What constitutes this diet is its plant-based cuisine using vegetables, fruits, cereals, nuts, and legumes, cooked with olive oil. In fact, the average Israeli individual has access to an average of 152 kilograms of fruits and 154 kilograms of vegetables each year. And thanks to Israeli culture, incorporating fresh salads into large breakfasts has effectively worked to suppress surges in blood sugar, facilitate weight loss, and avoid insulin resistance for diabetics. In other cases, this diet has been shown to prevent chronic and degenerative diseases as well.
Because of the diet’s emphasis on plant based foods for essential nutritional fibers, vitamins and minerals, people who follow it typically consume less fish, seafood, dairy, and particularly less red meat, thereby minimizing the consumption of saturated and trans fats and considerably improving cardiovascular health. Even when the diet was tested on patients who had previously suffered from heart attacks, the occurrence of acute coronary episodes was reduced by 50%. Plus, studies have revealed that the Mediterranean diet can be responsible for lowering instances of cancer mortality as well as avoiding most digestive cancers altogether.
The benefits of a Mediterranean diet are no novel phenomenon here in Israel. Rather, it has simply piqued scientist’s interest when it comes to individual gut health and personalized medicine and nutrition. Personalized medicine consists of tailored and specific medical treatments based on a patient’s individual characteristics. This differs from other sectors of medical treatment such that this approach relies on scientific breakthroughs in understanding a person’s unique molecular and genetic profile, helping healthcare providers predict the safest and perhaps most effective course of action for a specific patient.
With less than 105 diet-related deaths per 100,000 people, Israel has one of the lowest mortality rates when it comes to dietary risks, globally. However, this does not account for the obesity and nutrition imbalance that persists across the country. In fact, the prevalence of overweight and obesity in Israel is similar to those in other western countries, with about 23% of the adult population being obese.
Considering the pivotal impact diet has on one’s health, studies of the gut can be integral in determining how to improve personalized medicine and possibly revolutionize the field of nutritional health everywhere. At the Weizmann Institute of Science, researchers have dedicated their efforts to the microbiome of the gut, an ecosystem that is specific to each and every human being on the planet. With the hopes of making advances in the medical field, researchers are seeking out answers about nutrition that would provide personalized benefits for patients all the while being a sustainable option for the planet.
Sustainable Sustenance for the Stomach

Built on a broad variety of plants and animals while tending to ecological systems, a sustainable diet is one that embodies a low environmental impact compared to the impacts brought on by conventional agriculture systems. This means optimizing and making efficient use of natural resources to avoid wasteful tendencies, which often tend to deprive and pollute the environment. Beyond its benefits for improved gut health and personalized medicine, the Mediterranean diet certainly fits the bill when it comes to upholding sustainability.
The Food and Agriculture Organization (FAO) and International Center for Advanced Studies in Nutrition and Agriculture (CIHEAM) found that Mediterranean diet and its cultivation of foods from plant sources in fact qualifies as a sustainable diet.
The State of Israel harvests fresh produce in ways that take landscape, water usage, and waste products all into consideration. For example, legumes, a protein-rich food, uses far less land and water when compared to the inputs to harvest protein from animals. For instance, when it comes to worldwide agricultural land, nearly 60% is devoted solely to beef production, and this figure may very well grow as meat consumption is expected to rise by 76% by 2050.
Finite land aside, the amount of water it will take to satisfy current and projected demand is nothing short of outlandish. To produce just one metric ton of meat from chicken, pork, and goat, between 4,300 and 6,000 cubic meters of water are needed to supply to the animals. With beef, it’s much worse as an average of 15,400 cubic meters of water are required. Crops like vegetables or cereals, for example, only need 322 and 1,644 cubic meters of water per one metric ton.
In Israel, efforts to recycle wastewater and use it for farming land irrigation purposes lessens the environmental burden that would otherwise accompany the agriculture industry. As a result, foods that originate from plants create fewer pollutants and maintain biodiversity. In turn, Israeli’s have ample access to local, seasonal, and fresh food, allowing them to make sustainable choices regarding their meals almost by default.
The recent studies by the Weizmann Institute paired with the environmental benefits of the Mediterranean diet illustrate how the ecology of the gut and our Earth can both flourish.
That Gut Feeling

Lead by principal investigators Eran Elinav and Eran Segal, researchers at the Weizmann Institute of Science have examined individual-specific responses to diet and its relationship to the gut microbiome––the ecosystem of all the microorganisms involved in our digestive processes, from the mouth to anus. In order for many of these organisms to thrive, they rely on various nutrients and resources that humans consume from their regular diet. However, a person’s microbiome is also influenced by the composition, amount, and timing of their diet as well.
Because gut microbiota provide crucial benefits in the form of immune system development, prevention of infections, nutrient acquisition, and even the functionality of the brain and nervous system, it is not something to overlook. What’s more is that research also shows that it plays a causal role when it comes to developing pathologies of obesity, autoimmune diseases, and neurological diseases.
Although a large proponent of one’s gut health originates from genetically-inherited traits passed down from one generation to another, the dietary habits and choices we make are essential in establishing diversity of the gut microbiome in humans. A person’s metabolism, diet, and nutrition can outweigh genetic and environmental factors in determining health outcomes for certain conditions like diabetes, obesity, IBS (irritable bowel syndrome), IBD (inflammatory bowel disease), colorectal cancer, and depression. Therefore, when it comes to our health, it is just as important if not more so to consider the food we consume because our meals more effectively dictate the biology of our gut microbiome.
A Satisfying Scientific Discovery
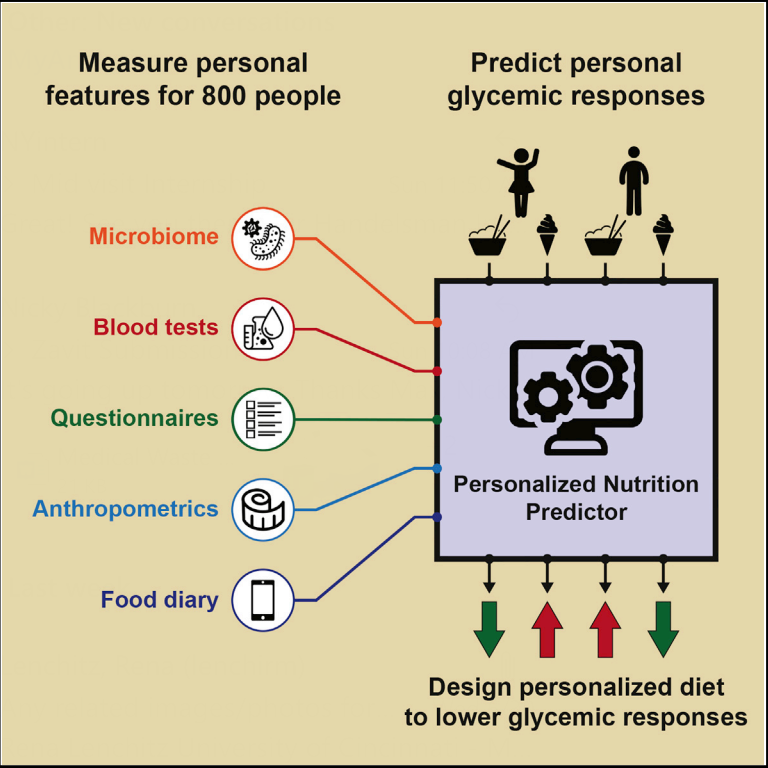
Because they have significant cardiovascular and diabetic health implications, blood sugar responses of an individual are crucial when determining treatment. With over 400 million people suffering worldwide from diabetes, predicting an individual’s response to food based on their lifestyle and microbiome could expedite successful medical intervention for pre-diabetic patients. To this end, Israeli researchers have discovered how a personalized dietary intervention tailored to an individual can substantially improve glycemic responses and parameters.
“Our research team had a cohort of about 800 individuals, and we wanted to study their reaction to postprandial––meaning after meals––glycemic responses to several foods. So, we created these standardized meals that consisted of specifically known amounts of calories and carbohydrates,” says Dr. Niv Zmora, MD and PhD from Prof. Eran Elinav’s lab at the Weizmann Institute. “We had each participant log their daily activities, meals, habits and medications for a period of one week. In the end, we analyzed the data and ultimately developed an algorithm to predict postprandial glycemic responses based on individual features.”
The results of their research are dependent on data collected from blood tests, anthropometrics, food diaries, and of course, their gut microbiome.
“Every person gave us a stool sample that we then analyzed and extracted DNA from to understand the composition of their gut microbiota. In the end, we had this algorithm that could predict postprandial glycemic responses more so than the methods used these days like carb counting or calorie counting,” says Dr. Zmora.
After validating the algorithm model, the last step was to devise a real-life menu for the individuals of the study, following up with them for a period of two weeks. One week they were given a ‘bad menu’, one that would induce high postprandial glycemic levels, followed by a ‘good menu’ which would induce mild glycemic responses.
“We saw that people were following our predictions, and we could monitor and maintain normal glycemia, meaning a normal blood glucose level for those following the ‘good menu.’ We also had great data to compare the two,” explained Zmora. This research was a cornerstone for personalized medicine efforts, laying the groundwork for personalized nutrition. By considering microbiome features, host characteristics, and dietary habits, scientists were able to integrate machine-learning algorithms to further understand how varying individual variability in their gut corresponded to their subsequent sugar levels.
The results of the studies have massive implications for the future prospects of personalized medicine, allowing physicians to predict responses that are tailored to the patient specifically.
“As physicians, we are used to this term personalized medicine, and it’s widely practiced. However, it’s still intriguing to see there hasn’t really been an application of personalized nutrition,” says Dr. Zmora. “This is kind of strange because food consists of nutrients, chemicals, and different components that we consume more often than we do medications. It doesn’t quite make sense that we don’t individualize nutrition.”
Not only could a personalized nutritional plan potentially increase patient compliance and prevent weight gain-weight loss, but it can also diminish the risk of evoking detrimental cardiometabolic health outcomes.
“The major contribution of this study will be to those who struggle to maintain their blood glucose levels in a normal range. This is really good information for pre-diabetics, diabetics, or those suffering from a metabolic condition,” he says. “In the future, we hope to identify the long-term consequences of the gut microbiota considerations for personalized nutrition. Going forward, we hope to expand beyond just metabolism and to explore implications of other pathological medical states like inflammatory states or cancer.”
“Although our study was limited to sugar levels, we think personalized medicine should also include lipid levels, protein metabolism, and other micronutrients. In the end, I think the vision is to be able to devise a comprehensive algorithm for many nutrients and corresponding conditions,” Dr. Zmora concludes.
Thus, the Institute’s findings indicate how health predictions based on one’s microbiome were accurate and clinically beneficial when it came to person-specific responses to certain foods. At the forefront of scientific discovery lies the gut microbiome, which can pioneer disease-specific treatments and therapies that are more successful and more individualized than current nutrition-counseling efforts.
In order to have a healthier and happier future, we should be conscious about the choices we make to cultivate foods in a sustainable fashion, cook meals that are specific to the individual, and consult with our healthcare providers about personalized nutrition.
This ZAVIT Article was also published in NoCamels on 30 Jun. 2021







